The Effect of Medial Branch Block for Low Back Pain in Elderly Patients
Article information
Abstract
Objective
The aim of this cross-sectional study was to evaluate the outcome of a medial branch block (MBB) in elderly patients to determine the factors associated with the degree of pain relief.
Methods
Fifty-six patients 75 years or older with MBB from January 2013 to July 2015 were classified into two groups by the degree of pain relief. The outcome of the MBB was evaluated according to clinical factors.
Results
A MBB was shown to be effective for 39 (69.6%) patients. Seventeen (30.4%) were categorized in the non-effective group. The two groups were significantly different in the history of previous lumbar spine surgery but had similar ages represented (p=0.019).
Conclusion
A MBB can be an effective minimally invasive intervention in elderly patients. Because the MBB seemed less effective for the patients who had a lumbar surgery, careful selection of the patients before performing a MBB is necessary to provide a higher success rate of pain relief.
INTRODUCTION
The term zygapophysial joints refers to the joints formed by the small growths that posteriorly bridge consecutive vertebrae. This term is often replaced by the term “facet joints”, an American neologism1). Various interventions that target the zygapophysial joint for the treatment of the pain have been referred to as facet joint injections. Among them, a medial branch block (MBB) is a local anesthetic block of the nerves that innervate a zygapophysial joint. In clinical trials MBBs has shown great validity in the control of chronic low back pain (LBP) or even acute LBP from facet joint dysfunction6). Therefore, MBB can be used as a useful alternative to surgical management for elderly patients whose surgical risk could be considerably high.
However, factors associated with the success rate of MBBs have not yet been established.
The aim of this study was to optimize the effect of a MBB in elderly patients by analyzing the possible factors associated with improvement.
MATERIALS AND METHODS
1. Study Population
This cross-sectional study was performed on all patients 75 years old and over who were admitted to our hospital from January 2013 to July 2015 for the treatment of back pain in the lumbar region. We enrolled patients with dynamic low back pain, which was documented to be aggravated with motion. The exclusion criteria were primary or metastatic spine tumor or spinal cord injury. Fifty-six consecutive patients were enrolled in our study. An institutional database was reviewed according to sex, age, past medical history and degree of pain relief. The presence of an osteoporotic compression fracture (OCF) of the spine was identified based on medical records, spine MRI and plain radiographs. The World Health Organization (WHO) classification system was used to define osteoporosis as a T-score ≤2.5 and osteopenia as 2.5 <T-score <1. Permission for approval was waived by our institutional review board.
2. Technique of Medial Branch Block
Under the guidance of fluoroscopy, the site of skin puncture was set at the junction of the most proximal portion of the transverse process and the superior articular process of the facet joint. Skin puncture was performed using a 22-gauge spinal needle advancing in an anteromedial direction until the tip of the needle is placed between the base of the transverse process and the superior articular process. The location of the needle tip was confirmed by a lateral fluoroscopic view of the lumbar spine. Then, 2 cc of the mixed anesthetic solution (0.5% bupivacaine hydrochloride 0.5 cc +dexamethasone 5 mg +normal saline 0.5 cc) was injected for the blockade of the medial branch.
3. Outcome Assessment
All patients who underwent a MBB for low back pain were followed up in the outpatient clinic at least two weeks after the first procedure. The degree of pain relief was graded from 1 to 4 in the following order: “Excellent” (improvement >75 %), “Good” (50–70%), “Fair” (25–50%), and “Poor” (<25 %). We defined the outcome of the MBB to be effective when the patients reported that the pain was relieved by more than 50%. These were classified as the “Excellent” or “Good” pain relief groups. Non-effective was defined as pain relief of less than 50%.
4. Statistical Analysis
Statistical analyses were performed using commercially available SPSS software, version 20.0 (IBM SPSS Inc., Armonk, NY, USA). For continuous variables, one-way analysis of variance was used. And, for categorical variables, Pearson’s Chi-squared or Fisher’s exact test was used. The outcomes of the MBB were also evaluated between the age groups using ANOVA methods. To find the prognostic factors related with the outcome of MBB, multivariable logistic regression analysis was used. Two-sided p values of <0.05 were assumed to be statistically significant.
RESULTS
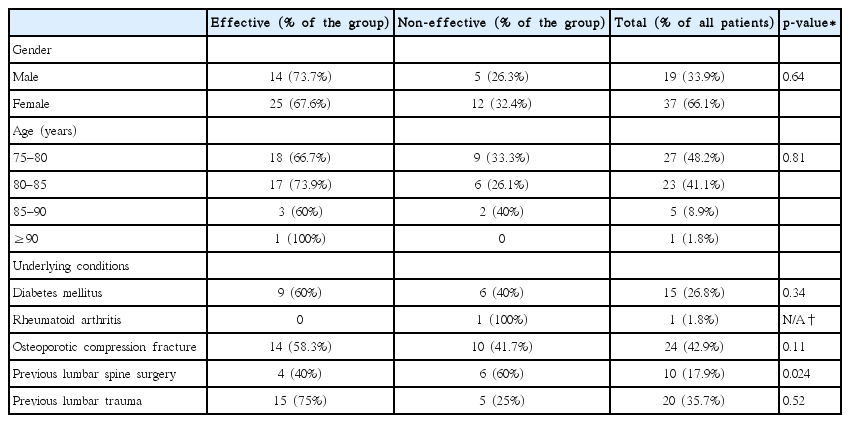
During the study period, 56 patients were treated with a MBB for low back pain. Of the study population, 37 were women and 19 were men. The clinical diagnoses before the MBB were for lumbar spondylosis in 54 patients and OCF of the lumbar spine in 24 patients. Thirty-four (60.7%) of the 56 patients were documented to have motion-related back pain in their medical records. The mean age of the patients was 80.11±3.93 years (range, 75 to 90 years). The demographics of the patients are listed in Table 1. The patients were divided into two groups based on the outcomes of the MBB. The MBB was shown to be effective for 39 (69.6%) patients. Seventeen (30.4%) were categorized in the non-effective group.
The effect of the MBB was assessed based on the patient’s clinical characteristics (Table 1). History of a previous lumbar spine surgery was the only factor that was significantly different between the effective and non-effective groups (p=0.019) (Table 2). The degree of pain relief that was graded from 1 to 4 based on each patient’s response was not significantly different between the age groups (Table 3).
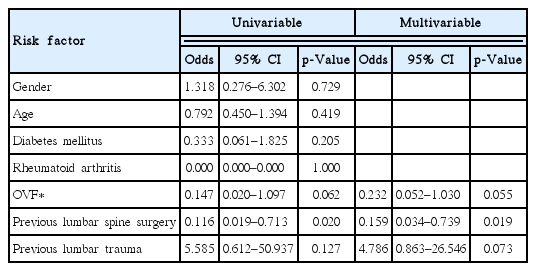
Logistic regression analysis for the potential parameters contributing to the outcome of medial branch block
DISCUSSION
The zygapophysial joint of the lumbar spine, which forms the posterolateral articulations to connect the vertebral arches, receives dual innervations from medial branches arising from the posterior primary rami at the same level and one level above the zygapophysial joint3). It has generally been accepted that the lumbar zygapophysial joint is a potential source of low back pain, especially facetogenic back pain. Blocks of the medial branches that innervate the zygapophysial joint have been recognized as being effective in alleviating patients’ motion-related chronic back pain3), rather than static back pain. Facet joint osteoarthritis becomes more prevalent with age. Of the community-based adults in the Framingham Heart Study, moderate or severe lumbar facet joint osteoarthritis on CT imaging was present in 36% of adults age <45 years, 67% of adults age 45–64 years, and 89% of those age 65 years and older16).
Therefore, a MBB could be an effective treatment modality for functional recovery and pain reduction in elderly patients with medical co-morbidities because it is less invasive and safer. However, to our knowledge, no study has demonstrated the effect of MBB and its associated clinical factors in elderly patients14).
In the literature, the rate of pain improvement after facet blocks or an MBB in patients with low back pain has been reported to be 29–60%10,11). In a recent study by Kim et al., approximately 70% of patients had pain relief to varying degrees9). In our series, 39 (69.6%) of the 56 patients have benefitted from MBBs for their low back pain.
Factors related to poor response to MBB have been investigated in previous studies. Kim et al. reported that long symptom duration (≥6 months), old age (≥60 years) and presence of radiating pain were associated with a poor prognosis after MBB in their study9). However, in the study by Rocha ID et al., the average age of patients who responded well to a MBB was significantly higher than that of the non-responding group4). However, in our study population of elderly patients, pain relief was not significantly different between the age groups.
Acute and old compression fractures are commonly incidentally observed in elderly patients with low back pain. Structural deformity of the vertebra after a compression fracture imposes more weight load on the facet joint, leads to facet joint arthritis and may contribute to pain12). Park et al. reported that a MBB provided patients with osteoporotic spinal compression fractures complaining of persistent low back pain significant pain relief (>40%), functional improvement (> 20%). In fact, 78.9% of their patients rated their satisfaction level as “excellent” or “good” 12 months after the first injection13).
In our series, the 24 (42.9%) out of 56 patients were identified to have osteoporotic compression fracture at admission that were proven by radiography. Among 24 patients, no one had acute compression fracture at the time of admission. All patients with the radiologically proven OCF did not undergo vertebroplasty. Some of them were incidentally found to have OCF in the radiographic evaluation for their back pain and the other patients with the OCF had managed conservatively for their OCF instead of vertebroplasty because their OCF were considered to stay stable with conservative management. We investigated the effectiveness of MBB in the patient with the radiologically proven OCF under the assumption that structural deformity of the vertebra after an OCF may lead to facet joint arthritis that can eventually provoke the pain because more weight load imposed on the facet joint. The 42.9% of the study population had OCFs of the lumbar spine. The improvement rate after the MBB was 58.3%, which was not significantly different from those without the OCF (p= 0.11). Because the previous study had the longer follow-up duration after MBB compared to that in the present study, the result of the present study may be different.
Minimally invasive interventional procedures have also been applied to failed back surgery syndrome, which is defined as persistent back pain despite having undergone spinal surgery of any type because the failure rate of the revision surgery is often high7,15).
Based on previous studies on the efficacy of a radiofrequency ablation (RFA) for facetogenic pain, Hussain et al. suggested that a RFA of the medial branch can be used for patients who have had previous surgery7). However, in our study population, the effect of the MBB was significantly lower in the patients with a history of previous lumbar surgery. In the present study, all enrolled patient were not related with failed back surgery syndrome. Because of that reason, it is difficult to compare the results of the previous and the present studies. In the future study with more number of patients, we will study the effect of failed back surgery syndrome on the outcome of MBB. And, the patients with persistent low back pain after lumbar surgery, who are suspected to have failed back surgery syndrome, may be ruled out from a RFA treatment because of the higher rate of negative results from MBBs.
Regarding the success of facet denervation, medial branch neurotomy using RFA has been evaluated in previous studies. In a large study by van Wijk et al., a 50% or greater decrease in the back pain was reported after a RFA of the lumbar facet joints in patients with chronic low back pain17).
Because the success of radiofrequency facet denervation is known to be dependent upon patient selection, a MBB can be used for diagnostic purposes to select patients with facet joint pain from a nonspecific low back pain patients18).
The International Spine Intervention Society (ISIS) recommended that lumbar medial branch radiofrequency neurotomy should only be considered if there is at least 80% relief after 2 diagnostic MBBs, considering the high false-positive rate of a single MBB2,5).
The limitation of our study is that the duration of pain relief was not evaluated individually and the number of MBBs either for diagnostic purposes or the treatment of the pain was not considered in the assessment of the outcome of the MBBs. Theoretically, an injection of a local anesthetic on the medial branch nerve in patients with facetogenic pain can only be expected to provide pain relief for the duration of the local anesthetic. Pain relief that lasts longer than this expected time period is likely due either to relief through natural history or, more likely, a placebo effect8). Therefore, further clinical trials regarding the effect of MBBs should be placebo-controlled. And, another limitation of this study is the history of pain medication in each individual was not investigated in our study, which may act as a confounding to affect the result of pain relief after the MBB
CONCLUSION
A MBB can be an effective intervention in elderly patients. Because the MBB seemed less effective for the patients who had a lumbar surgery, careful selection of the patients before performing a MBB is necessary to provide a higher success rate of pain relief.